Rotablation (Rotational Atherectomy): A Detailed Guide to the Procedure
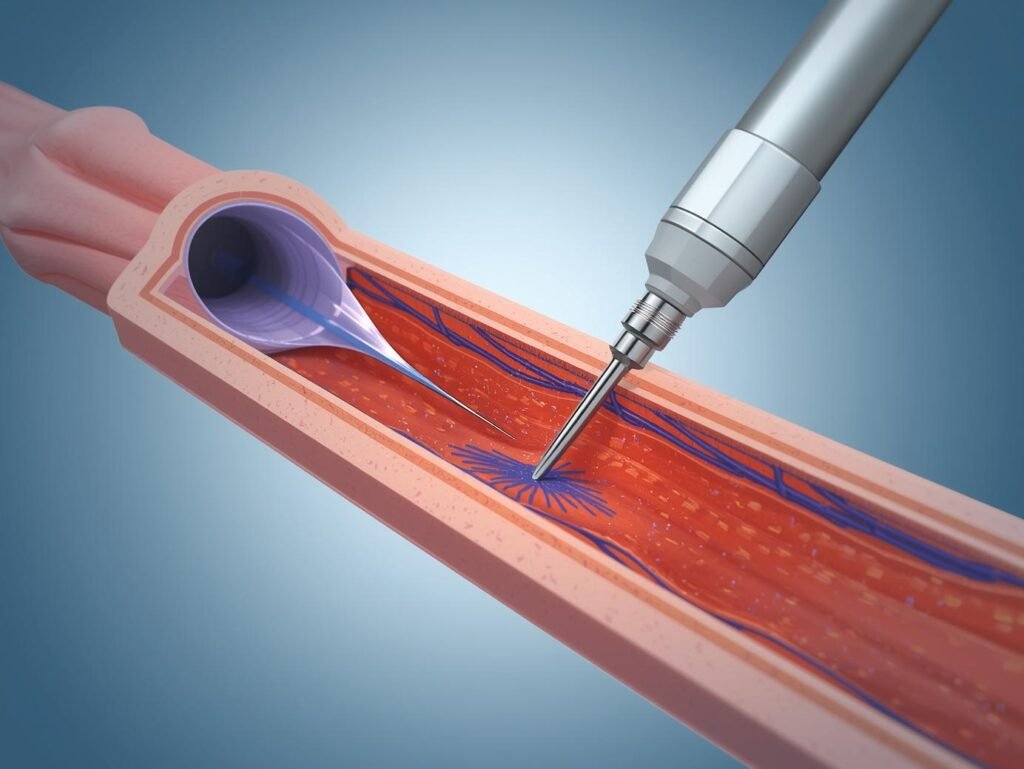
Coronary artery disease (CAD) occurs when cholesterol, fat, and calcium deposits build up inside the coronary arteries. Over time, these deposits harden, causing severe blockages that restrict blood flow to the heart. Treating such calcified blockages can be challenging with regular angioplasty alone. This is where Rotablation, also called Rotational Atherectomy, plays a key role.
What is Rotablation?
Rotablation is a specialized technique used during angioplasty to treat severely calcified and hardened plaques in the coronary arteries. Instead of simply pushing the blockage aside (like balloon angioplasty does), Rotablation uses a high-speed diamond-tipped burr that rotates at speeds up to 200,000 revolutions per minute (rpm).
The rotating burr grinds down the hard calcium into microscopic particles (smaller than red blood cells), which safely pass through the bloodstream and are filtered out by the body. This process modifies the plaque, softens the vessel, and allows balloons and stents to expand properly.
Why is Rotablation Needed?
Rotablation is usually recommended when:
- The artery is heavily calcified and cannot be opened with balloons.
- A stent cannot be delivered or expanded due to the hardness of the plaque.
- The lesion is uncrossable or undilatable using standard PCI techniques.
- Patients have undergone a failed angioplasty attempt.
In short, Rotablation is reserved for difficult cases where conventional methods are not enough.
Step-by-Step Rotablation Procedure
1. Patient Preparation
- The procedure is performed in a cardiac catheterization lab (cath lab).
- Patients are given local anesthesia at the access site (usually wrist or groin).
- Sedation may be given, but patients are generally awake.
- Continuous monitoring of heart rhythm, oxygen, and blood pressure is done.
2. Arterial Access
- A sheath (small tube) is inserted into the radial artery (wrist) or femoral artery (groin).
- Through this, catheters and guidewires are passed into the coronary arteries.
3. Guidewire Placement
- A special guidewire designed for Rotablation (called a RotaWire) is positioned across the blockage.
- Correct positioning is crucial to ensure safety and efficiency.
4. Insertion of the Rotablator
- The Rotablator device, with its diamond-coated burr, is advanced over the guidewire to reach the calcified lesion.
- The burr comes in different sizes (1.25–2.0 mm), and the cardiologist selects the appropriate one depending on artery size.
5. Plaque Modification (Atherectomy)
- The burr is activated and begins spinning at up to 200,000 rpm.
- The cardiologist gently advances and withdraws the burr in short, controlled runs (“pecking motion”).
- This technique gradually grinds the calcified plaque into micro-particles, without generating heat or large debris.
6. Balloon Angioplasty
- After the calcium is modified, a balloon catheter is inserted and inflated to widen the artery.
- This step ensures the artery is soft enough for stent deployment.
7. Stent Placement
- A stent (metal mesh tube) is then carefully placed in the artery.
- Because of Rotablation, the stent expands properly, reducing the risk of restenosis (re-narrowing).
8. Final Checks & Completion
- The cardiologist performs a final angiogram to ensure blood flow is restored.
- The catheter and sheath are removed, and pressure or closure devices are applied to the access site.
- The patient is moved to a recovery area for observation.
The entire procedure typically lasts 60–90 minutes, depending on the complexity of the blockage.
What Happens to the Plaque Particles?
The plaque is reduced into microscopic particles (<5 microns)—smaller than red blood cells. These tiny fragments are safely carried away in the bloodstream and filtered by the liver and kidneys, without causing harm.
Benefits of Rotablation Procedure
- Makes balloon angioplasty and stent placement possible in hardened arteries.
- Improves chances of long-term stent success.
- Provides immediate symptom relief from angina.
- Minimally invasive, avoiding open-heart surgery.
- Allows treatment of complex, high-risk patients.
Risks of the Procedure
While generally safe in experienced hands, Rotablation carries certain risks:
- Temporary slowing of blood flow (no-reflow).
- Damage to artery walls (dissection or perforation).
- Irregular heart rhythms during the procedure.
- Rarely, heart attack or stroke.
- Bleeding at the access site.
Cardiologists use advanced imaging like IVUS (Intravascular Ultrasound) or OCT (Optical Coherence Tomography) to plan and guide the procedure, minimizing risks.
Recovery After Rotablation
- Most patients are kept overnight for observation.
- Light activities can be resumed in 2–3 days.
- Medications such as antiplatelets, statins, and beta-blockers are continued.
- Lifestyle changes (diet, exercise, smoking cessation) are essential to prevent further blockages.
Conclusion
Rotablation (Rotational Atherectomy) is a cutting-edge procedure designed to tackle hard, calcified coronary artery blockages that standard angioplasty cannot manage. By modifying the plaque and enabling proper stent placement, it restores blood flow to the heart and reduces the risk of future complications.
If you have been told that your coronary arteries are too calcified for regular angioplasty, Rotablation may be the right treatment option. Speak to an experienced interventional cardiologist to understand whether this advanced procedure is suitable for you.

